Pacemaker powered by light eliminates need for batteries and allows the heart to function more naturally—new research
Powered by WPeMatico
Powered by WPeMatico

Canada: A recent study published in Radiology: Cardiothoracic Imaging has suggested that current and former smoking status are independently associated with low coronary volume-to-myocardial mass ratio (V/M) on CT fractional flow reserve (CT-FFR).
“Smoking is associated with lower coronary volume-to-myocardial mass ratio in individuals with coronary artery disease (CAD),” the researchers reported. The findings further cement the link between smoking and heart disease.
Current and former smoking were independently associated with lower V/M in participants with coronary artery disease, the researchers noted.
Previous studies have shown that a low volume-to-myocardial mass ratio is associated with conditions such as hypertrophic cardiomyopathy microvascular angina, and coronary artery disease, with greater stenosis. However, the effect of smoking volume-to-myocardial mass ratio has not been thoroughly established. To fill this knowledge gap, Kenneth R. Holmes, University of British Columbia, Vancouver, BC, Canada, and colleagues aimed to investigate the relationship between smoking status and coronary V/M among individuals with CAD undergoing CT fractional flow reserve analysis.
The secondary analysis included participants from the ADVANCE registry evaluated for suspected CAD from 2015 to 2017, who were found to have coronary stenosis of 30% or a greater at coronary CT angiography (CCTA) if they had known smoking status and underwent CT-FFR and V/M analysis.
CCTA images were segmented to calculate myocardial mass and coronary volume. V/M was compared between smoking groups, and predictors of low V/M were determined.
The sample for analysis consisted of 503 current smokers, 1060 former smokers, and 1311 never-smokers (2874 participants; 1906 male participants).
The study led to the following findings:
In conclusion, history of smoking (current or former smoking status) was an independent predictor of low V/M derived from CT-FFR,
“Mechanisms driving low V/M in smokers and the potential use of V/M as a surrogate marker of vascular health and predictor of downstream clinical outcomes require further study.
Reference:
Holmes KR, Gulsin GS, Fairbairn TA, Hurwitz-Koweek L, Matsuo H, Nørgaard BL, Jensen JM, Sand NR, Nieman K, Bax JJ, Pontone G, Chinnaiyan KM, Rabbat MG, Amano T, Kawasaki T, Akasaka T, Kitabata H, Rogers C, Patel MR, Payne GW, Leipsic JA, Sellers SL. Impact of Smoking on Coronary Volume-to-Myocardial Mass Ratio: An ADVANCE Registry Substudy. Radiol Cardiothorac Imaging. 2024 Apr;6(2):e220197. doi: 10.1148/ryct.220197. PMID: 38483246.
Powered by WPeMatico
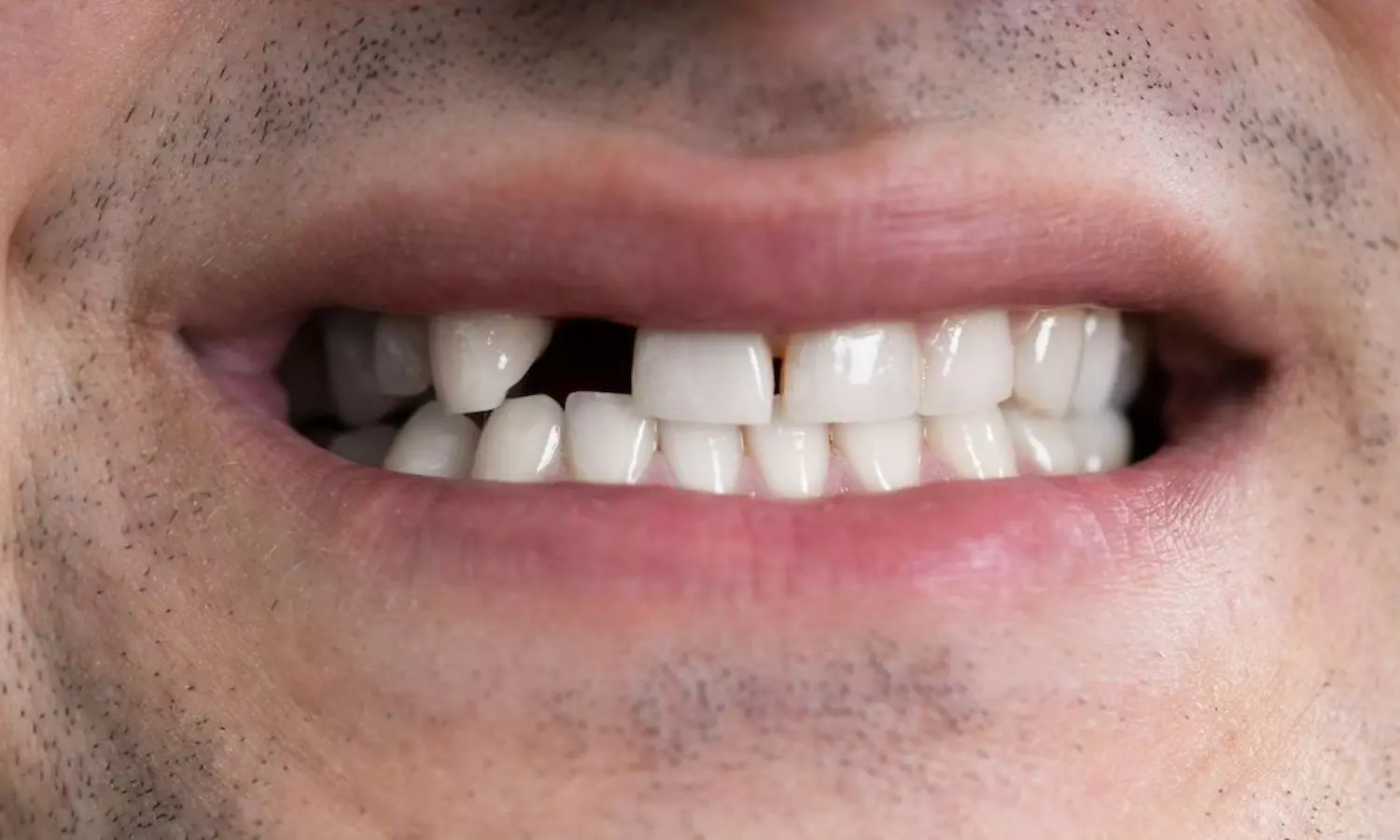
Denmark: A recent study published in JAMA Network Open has suggested an association between tooth agenesis and specific cancer types, specifically in childhood and early adulthood.
“Our population-based cohort study of 2.5 million live-born singletons with up to 40 years of follow-up showed that tooth agenesis was positively associated with several cancer types, including nephroblastoma, neuroblastoma, and hepatoblastoma in childhood; osteosarcoma in adolescence; and carcinomas of the bladder and colorectal carcinomas in young adulthood,” the researchers reported.
Previous studies have provided some evidence that tooth agenesis (congenital absence of one or more teeth) is associated with cancer risk, particularly carcinomas of the ovaries and colon, but these results are conflicting, and associations have not been evaluated yet in a population-based setting. To fill this knowledge gap, Saga Elise Eiset, Department of Clinical Medicine, Aarhus University, Aarhus, Denmark, and colleagues aimed to investigate the association between tooth agenesis and specific cancer types before 40 years of age.
For this purpose, the researchers used linking data from nationwide registries in Denmark to evaluate all Danish live-born singletons born from 1977 to 2018 and followed for up to 4 years. Data analysis was done from January through June 2023.
Exposure was tooth agenesis as documented by the Danish Central Registry of Odontology from 1988 to 2018, and from hospital encounters in the Danish National Patient Registry within the entire study period.
The study’s primary outcome was the first cancer diagnosis before 40 years of age obtained from the Danish Cancer Registry. Cox proportional hazards regression as hazard ratios (HRs) estimated associations between tooth agenesis and specific cancers.
Analyses were divided into age groups: younger than 1 year, 1 to younger than three years, 3 to younger than 10 years, 10 to younger than 20 years, 20 to younger than 30 years, and 30 to younger than 40 years. After excluding individuals with known syndrome, associations with nonsyndromic tooth agenesis were evaluated.
The study led to the following findings:
In conclusion, the cohort study supports previous evidence indicating an association between tooth agenesis and the risk of colorectal cancer in early adulthood. The findings also suggest associations with several other specific cancer types, in particular, extracranial embryonal tumors in childhood. However, within the study period, there was a low absolute number of tooth agenesis–cancer co-occurrences.
“An improved understanding of the genetic causes of the specific associations is needed to assess possible clinical implications,” the researchers wrote.
Reference:
Eiset SE, Schraw J, Sørensen GV, et al. Congenital Tooth Agenesis and Risk of Early-Onset Cancer. JAMA Netw Open. 2024;7(3):e240365. doi:10.1001/jamanetworkopen.2024.0365
Powered by WPeMatico

France: A recent study published in the Journal of Sleep Research has shown that atypical deglutition (tongue thrust) is associated with more severe apnea in children with obstructive sleep apnea syndrome (OSAS). Atypical deglutition was more strongly associated with altered facial measurements and increased pharyngeal collapsibility in children.
The findings suggest that identifying atypical deglutition in children with OSAS could help to guide a personalized therapeutic approach, including myofunctional therapy.
Previous studies have proposed a link between atypical deglutition and pediatric obstructive sleep apnea syndrome and that its correction through myofunctional therapy could potentially ameliorate OSAS symptoms. The role of myofunctional therapy in managing pediatric OSAS remains debatable. Plamen Bokov, INSERM NeuroDiderot, Paris, France, and colleagues aimed to assess the prevalence of atypical deglutition in children diagnosed with moderate to severe OSAS and to explore its associations, particularly concerning the type of dentition (mixed or permanent).
For this purpose, the researchers conducted a study over 5 years at a pediatric hospital in Paris, France. It included children aged 6–18 years with moderate to severe OSAS (apnea–hypopnea index ≥5/h) who underwent a comprehensive evaluation, including the symptoms of snoring and breathing issues, recording of demographic data, and otolaryngology examination.
The swallowing pattern was evaluated, and orthodontic evaluations were performed. The researchers conducted cophalometric radiography and pharyngometry tests (pharyngeal collapsibility was computed).
The researchers reported the following findings:
In conclusion, in children with moderate to severe OSAS diagnosis, the presence of atypical deglutition is associated with increased pharyngeal collapsibility and a more severe apnea–hypopnea index, as well as with distinctive facial features, characterized by increased proportions of the lower part of the face and a lower position of the hyoid bone.
“Thus, it is crucial to recognize atypical deglutition as a potential risk factor contributing to the severity of OSAS in children,” the researchers wrote. Consequently, they recommend considering early intervention through myofunctional therapy as a viable treatment approach.
Reference:
Bokov, P., Dahan, J., Boujemla, I., Dudoignon, B., & Delclaux, C. The role of atypical deglutition in children and adolescents with moderate to severe obstructive sleep apnea syndrome. Journal of Sleep Research, e14175. https://doi.org/10.1111/jsr.14175
Powered by WPeMatico

Keloids are abnormal growths of scar tissue that can form at the site of a wound or injury. Triamcinolone acetate injections are commonly used to treat keloids, but some cases do not respond well to this treatment or experience recurrence. Recently, intralesional bleomycin has shown promising results in keloid treatment.
Triamcinolone acetate injections are a standard treatment for keloids, but their efficacy varies, and recurrence rates can be high. Intralesional bleomycin has emerged as a potential alternative, but its effectiveness in combination with triamcinolone remains uncertain.
A recent study aimed to evaluate the efficacy of combining bleomycin and triamcinolone for refractory keloids. This study was published in the journal of Dermatologic Surgery by Mozafari and colleagues. A total of 33 patients with resistant keloids were enrolled in the study. They received a mixture of bleomycin (1 u/cc) and triamcinolone acetonide (13.3 mg/cc) injected intralesionally every 4 to 6 weeks for up to 6 cycles. The Japan Scar Scale (JSS) and physician’s global assessment were used to evaluate clinical improvement, and side effects were recorded.
The key findings of the study were:
• The study included 33 patients (8 men, 25 women) with a mean age of 36.52 years.
• After treatment, all patients showed a significant decrease in total JSS scores compared to baseline (p < .001). 26 keloids (78.8%) exhibited excellent response (75%–100% flattening), 7 keloids (21.2%) showed fair response (25%–75% flattening), and none showed poor response (<25% flattening)
• Side effects included ulceration (33.3%), hyperpigmentation (33.3%), hypopigmentation (15.15%), secondary infection (33.3%), and telangiectasia (15.15%).
The combination of bleomycin and triamcinolone proved to be effective in treating refractory keloids, with the majority of patients showing significant improvement. This therapy offers a promising option for individuals who have not responded well to traditional treatments. However, side effects such as ulceration and hyperpigmentation were observed and should be monitored closely during treatment.
Reference:
Powered by WPeMatico

Ketone monoester drink reduces postprandial blood sugar in adults with type 2 diabetes, finds randomised controlled trial suggests a new study published in the Diabetologia.
The present study aimed to conduct a randomised, placebo-controlled, double-blind, crossover trial to determine whether pre-meal ketone monoester ingestion reduces postprandial glucose concentrations in individuals with type 2 diabetes. In this double-blind, placebo-controlled, crossover design study, ten participants with type 2 diabetes (age 59±1.7 years, 50% female, BMI 32±1 kg/m[2], HbA1c 54±2 mmol/mol [7.1±0.2%]) were randomised using computer-generated random numbers. The study took place at the Nutritional Physiology Research Unit, University of Exeter, Exeter, UK. Using a dual-glucose tracer approach, we assessed glucose kinetics after the ingestion of a 0.5 g/kg body mass ketone monoester (KME) or a taste-matched non-caloric placebo before a mixed-meal tolerance test. The primary outcome measure was endogenous glucose production. Secondary outcome measures were total glucose appearance rate and exogenous glucose appearance rate, glucose disappearance rate, blood glucose, serum insulin, β-OHB and NEFA levels, and energy expenditure. RESULTS: Data for all ten participants were analysed. KME ingestion increased mean ± SEM plasma beta-hydroxybutyrate from 0.3±0.03 mmol/l to a peak of 4.3±1.2 mmol/l while reducing 2 h postprandial glucose concentrations by ~18% and 4 h postprandial glucose concentrations by ~12%, predominately as a result of a 28% decrease in the 2 h rate of glucose appearance following meal ingestion (all p<0.05). The reduction in blood glucose concentrations was associated with suppressed plasma NEFA concentrations after KME ingestion, with no difference in plasma insulin concentrations between the control and KME conditions. Postprandial endogenous glucose production was unaffected by KME ingestion (mean ± SEM 0.76±0.15 and 0.88±0.10 mg kg[-1] min[-1] for the control and KME, respectively). No adverse effects of KME ingestion were observed. KME ingestion appears to delay glucose absorption in adults with type 2 diabetes, thereby reducing postprandial glucose concentrations. Future work to explore the therapeutic potential of KME supplementation in type 2 diabetes is warranted.
Reference:
Monteyne, Alistair J., et al. “A Ketone Monoester Drink Reduces Postprandial Blood Glucose Concentrations in Adults With Type 2 Diabetes: a Randomised Controlled Trial.” Diabetologia, 2024.
Keywords:
Ketone monoester drink, postprandial, blood sugar, adults, type 2 diabetes, randomised controlled trial, Diabetologia, Monteyne, Alistair J
Powered by WPeMatico
USA: A recent study has suggested that decreased circulating monocytes are associated with reduced lung function and uniquely distinguish late-resolving COVID-pulmonary fibrosis (PF) from early-resolving COVID-PF, idiopathic pulmonary fibrosis (IPF), and non-diseased controls.
The findings, published in Frontiers in Immunology, could help doctors better personalize treatments for individual patients. The discovery will provide doctors with a useful tool to identify COVID-19 patients at risk for long-haul lung problems and help guide them to recovery.
UVA Health researchers have discovered a potential way to predict which patients with severe COVID-19 are likely to recover well and which are likely to suffer “long-haul” lung problems.
UVA’s new research also alleviates concerns that severe COVID-19 could trigger relentless, ongoing lung scarring akin to the chronic lung disease known as idiopathic pulmonary fibrosis, the researchers report. That type of continuing lung damage would mean that patients’ ability to breathe would continue to worsen over time.
“We are excited to find that people with long-haul COVID have an immune system that is different from people who have lung scarring that doesn’t stop,” said researcher Catherine A. Bonham, MD, a pulmonary and critical care expert who serves as scientific director of UVA Health’s Interstitial Lung Disease Program. “This offers hope that even patients with the worst COVID do not have progressive scarring of the lung that leads to death.”
Up to 30% of patients hospitalized with severe COVID-19 continue to suffer persistent symptoms months after recovering from the virus. Many of these patients develop lung scarring-some early on in their hospitalization, and others within six months of their initial illness, prior research has found. Bonham and her collaborators wanted to better understand why this scarring occurs, to determine if it is similar to progressive pulmonary fibrosis and to see if there is a way to identify patients at risk.
To do this, the researchers followed 16 UVA Health patients who had survived severe COVID-19. Fourteen had been hospitalized and placed on a ventilator. All continued to have trouble breathing and suffered fatigue and abnormal lung function at their first outpatient checkup.
After six months, the researchers found that the patients could be divided into two groups: One group’s lung health improved, prompting the researchers to label them “early resolvers,” while the other group, dubbed “late resolvers,” continued to suffer lung problems and pulmonary fibrosis.
Looking at blood samples taken before the patients’ recovery began to diverge, the UVA team found that the late resolvers had significantly fewer immune cells known as monocytes circulating in their blood. These white blood cells play a critical role in our ability to fend off disease, and the cells were abnormally depleted in patients who continued to suffer lung problems compared both to those who recovered and healthy control subjects.
Further, the decrease in monocytes correlated with the severity of the patients’ ongoing symptoms. That suggests that doctors may be able to use a simple blood test to identify patients likely to become long-haulers — and to improve their care.
“About half of the patients we examined still had lingering, bothersome symptoms and abnormal tests after six months,” Bonham said. “We were able to detect differences in their blood from the first visit, with fewer blood monocytes mapping to lower lung function.”
The researchers also wanted to determine if severe COVID-19 could cause progressive lung scarring as in idiopathic pulmonary fibrosis. They found that the two conditions had very different effects on immune cells, suggesting that even when the symptoms were similar, the underlying causes were very different. This held even in patients with the most persistent long-haul COVID-19 symptoms. “Idiopathic pulmonary fibrosis is progressive and kills patients within three to five years,” Bonham said. “It was a relief to see that all our COVID patients, even those with long-haul symptoms, were not similar.”
Because of the small number of participants in UVA’s study, and because they were mostly male (for easier comparison with IPF, a disease that strikes mostly men), the researchers say larger, multi-center studies are needed to bear out the findings. But they are hopeful that their discovery will provide doctors a useful tool to identify COVID-19 patients at risk for long-haul lung problems and help guide them to recovery.
“We are only beginning to understand the biology of how the immune system impacts pulmonary fibrosis,” Bonham said. “My team and I were humbled and grateful to work with the outstanding patients who made this study possible.”
Reference:
Grace C. Bingham, Chaofan Li, Yong Huang, Shwu-Fan Ma, Imre Noth, Jie Sun, High-dimensional comparison of monocytes and T cells in post-COVID and idiopathic pulmonary fibrosis, Frontiers in Immunology, https://doi.org/10.3389/fimmu.2023.1308594.
Powered by WPeMatico
In the realm of abortion care, the debate over cervical preparation methods for Dilation and Evacuation (D&E) procedures has taken center stage. This retrospective cohort analysis aimed to compare the efficacy and safety of two approaches: osmotic dilators plus same-day misoprostol versus overnight mifepristone. Overnight mifepristone proves to be a safe and effective alternative, potentially enhancing clinic flow and patient experience. The study found procedure time to be longer with adjunctive mifepristone compared to misoprostol; however, this difference is unlikely to be clinically meaningful. Furthermore, the frequency of acute complications was similar between groups
This study was published in the journal Contraception by Stephanie Lambert and colleagues. The study conducted at an ambulatory health center, the study included 664 patients initiating abortion between 18 and 22 weeks. The primary outcome was procedure time, with secondary safety outcomes including acute complications and bleeding complications.
The key findings of the study were:
Procedure Time:
Mifepristone group exhibited a higher mean procedure time (9.7±5.3 minutes vs. 7.9±4.4, p=0.004).
The difference, though statistically significant, did not reach clinical significance after adjustments.
Additional Medications:
Additional misoprostol usage was more common in the mifepristone group.
The use of an additional set of dilators did not differ between the groups.
Acute Complications:
Similar frequency of acute complications in the misoprostol (4.1%) and mifepristone (4.3%) groups (p=0.90).
While mifepristone prolonged procedure time, the difference was deemed clinically insignificant. Notably, acute complications demonstrated no significant variation between the two methods. This study’s insights advocate for the adoption of overnight mifepristone as a viable cervical preparation strategy for Dilation and Evacuation (D&E), offering a balanced perspective on efficacy, safety, and patient-centric considerations.Overnight mifepristone at the time of cervical dilator placement is a safe and effective alternative to adjuvant same-day misoprostol for cervical preparation prior to Dilation and Evacuation (D&E) and may offer benefits for clinic flow and patient experience.
Reference:
Lambert, S. J., Lunde, B., Porsch, L., Stoffels, G., MacIsaac, L., Dayananda, I., & Dragoman, M. V. Adjuvant misoprostol or mifepristone for cervical preparation with osmotic dilators before dilation and evacuation. Contraception,2024;110364:110364. https://doi.org/10.1016/j.contraception.2024.110364
Powered by WPeMatico
Recently published study investigated the association between plasma CA-125 levels and post-extubation respiratory failure (PERF) in critically ill patients. A prospective cohort study was conducted in a tertiary hospital, enrolling patients aged 18 years or older who had received mechanical ventilation (MV) for at least 48 hours. The study found that among the 103 enrolled patients, 44 (51.2%) experienced PERF, with 23 receiving non-invasive ventilation and 16 requiring reintubation within 72 hours. Patients who experienced respiratory failure showed significantly higher median CA-125 values compared to those without respiratory failure. The area under the ROC curve for CA-125 in predicting respiratory failure occurrence was 0.663, and CA-125 levels exceeding 35.0 U/mL were found to be significantly associated with the occurrence of respiratory failure in a logistic regression model. A post-hoc analysis combining CA-125 and lung ultrasound (LUS) scores showed an 81.0% incidence of respiratory failure in patients with elevated CA-125 and LUS scores, while patients with normal CA-125 and LUS scores had a markedly lower incidence of 32.0% for respiratory failure. The study suggests the potential utility of incorporating CA-125 into routine congestion assessments and reveals a potential role for combining CA-125 with LUS scores to evaluate a patient’s risk of developing PERF. The authors concluded that elevated CA-125 levels were associated with a higher incidence of respiratory failure among critically ill patients who were extubated following successful spontaneous breathing trials. The study highlighted the potential application of CA-125 in assessing and predicting respiratory outcomes in critically ill patients, particularly in the context of extubation. The findings hold implications for clinical practice, indicating the need for further research and potential incorporation of CA-125 into routine assessment protocols for critically ill patients in intensive care units.
Reference –
Lombuli, F., Montes, T.H.M. & Boniatti, M.M. Association between CA-125 and post-extubation respiratory failure: a cohort study. Crit Care 28, 31 (2024). https://doi.org/10.1186/s13054-024-04806-5
Powered by WPeMatico
China: A prospective community-based cohort study published in the International Journal of Cardiology has shed light on the relationship between resting heart rate and long-term outcomes in stabilized patients with myocardial infarction (MI).
The study showed that resting heart rate (RHR) during the stable phase after MI was independently associated with the primary outcome, all-cause death, and hospitalization for heart failure but not with recurrent MI and stroke in post-MI patients. RHR >72 bpm was associated with increased risk for primary outcome and all-cause death in patients with MI.
Resting heart rate during hospitalization is associated with negative outcomes in patients with myocardial infarction. Shouling Wu, North China University of Science and Technology, Tangshan, China, and colleagues aimed to evaluate the long-term prognostic effect of RHR during the stable phase after MI in post-MI patients.
The study enrolled patients with prior or new-onset MI and RHR measurements during the stable period after MI between 2006 and 2018 in the community-based Kailuan Study. Resting heart rate was categorized into four groups based on quartiles. The association of RHR with primary composite outcome of all-cause death, hospitalization for heart failure, stroke, and recurrent MI and its components, was analyzed using Cox regression analysis.
The study included 4447 post-MI patients. During a median follow-up of 7.5 years, 1813 patients developed primary outcomes.
The study revealed the following findings:
The study showed that resting heart rate during the stable phase after myocardial infarction was an independent predictor for primary outcome and all-cause death in post-MI patients.
“We found that resting heart rate >72 bpm was associated with an increased risk for the primary outcome and all-cause death in patients with MI,” the researchers wrote.
RHR reduction in patients with RHR >72 bpm is required to be studied in prospective trials to ascertain if it would reduce adverse outcomes in post-MI patients, they suggested.
Reference:
Xu L, Chen Y, Chen S, Wang G, Fu Y, Cai J, Yang X, Wu S, Miao C, Hong J. Relationship between resting heart rate and long-term outcomes in stabilized patients with myocardial infarction: A prospective community-based cohort study. Int J Cardiol. 2024 Jan 24:131811. doi: 10.1016/j.ijcard.2024.131811. Epub ahead of print. PMID: 38278489.
Powered by WPeMatico
